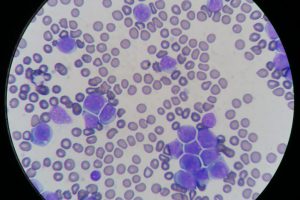
Blood smear evaluation is an often overlooked but a very important aspect for in-house haematology. With the advancement in haematology analysers that can now detect reticulocytes and even band neutrophils, some practitioners are beginning to rely solely on the numerical data alone in evaluating the patient’s blood. The art of blood smear interpretation is on the decline. However, it is an extremely valuable skill that needs to be practiced and perfected and should be part of every in-house haematology.
What are the benefits of understanding blood smears?
Blood smear evaluation begins with becoming accomplished at producing great diagnostic smears – this of course takes practice. Poorly performed smears can be non-diagnostic and frustrating to assess for both yourself and an external pathologist.
A few tips on the technique: